AI medical diagnosis accuracy is on the brink of transformation by 2026.
Innovative technology will enable doctors to reduce mistakes by a large margin. Robots and computers are now helping medical professionals. They will analyze test results and images with greater speed and accuracy. This teamwork will make diagnoses more accurate. This will save lives.
Each year, around 12 million Americans deal with diagnostic errors. These mistakes can delay treatment. They can also lead to preventable deaths. AI for medical diagnosis is advancing at a rapid pace. It provides solutions that are impressive.
Hospitals around the world are using AI now. This technology helps find cancers early and spot rare diseases fast. It also supports doctors in making better choices. The technology is operational and effective, and it has a positive impact on lives.
In this article, you study how AI and medical diagnosis are changing healthcare. Explore the wins and hurdles for patients and healthcare workers. Also, consider what comes next. Plus, discover the best free AI for medical diagnosis available today.
Medicine Meets Machine: How AI Is Redefining Diagnosis

A doctor spends years studying the human body. An AI can analyze millions of medical records in seconds. When these two forces combine, something extraordinary happens.
AI in healthcare uses machine learning algorithms to identify patterns in medical data, patterns that can be invisible to even the most experienced physician. These systems are trained on massive datasets of X-rays, MRI scans, lab results, and patient histories. Over time, they get better at spotting anomalies.
Think of it like spell-check, but for your health. Just as spell-check catches errors you might miss while writing, AI catches subtle signals in your medical data that could indicate a serious condition early on.
By 2026, AI-assisted diagnosis is no longer an experimental feature in elite research hospitals. It’s becoming standard practice. According to a report by Accenture, AI applications in healthcare could generate $150 billion in annual savings for the US economy by 2026, and diagnostic AI is one of the biggest contributors.
This shift is reshaping the patient experience from the ground up.
Traditional Diagnosis Has Limits: AI Is Here to Fill Them
Even skilled doctors miss things. It’s not a failure of intelligence; it’s a limitation of human capacity.
A radiologist reviewing hundreds of scans per day will inevitably experience fatigue. A general practitioner with a 15-minute consultation window can’t always catch a rare condition on the first visit. These aren’t excuses; they’re realities of an overburdened healthcare system.
Did You Know? Studies suggest that diagnostic errors contribute to approximately 40,000–80,000 deaths annually in the United States alone.
AI doesn’t get tired. It doesn’t have off days. It processes information with the same precision at 11 p.m. as it does at 9 a.m. And crucially, it can cross-reference a single patient’s data against millions of similar cases in real time, something no human doctor could physically do.
This doesn’t mean doctors are becoming obsolete. It means they’re getting a powerful second opinion, one that never sleeps and never skips a detail.
How AI Algorithms Are Supercharging Medical Diagnosis

Behind every AI diagnosis tool is a set of algorithms trained to find meaning in complex data.
The most widely used approach is deep learning, a type of machine learning that mimics how the human brain processes information. When applied to medical imaging, deep learning models can analyze pixel-by-pixel details in an X-ray or MRI scan and flag areas of concern with pinpoint accuracy.
Natural Language Processing (NLP) is another major tool. It allows AI systems to read and interpret unstructured clinical notes, doctor reports, and patient histories, extracting useful diagnostic insights from text that would otherwise take hours to review manually.
Then there’s predictive analytics. By analyzing patterns across large patient populations, AI can predict who is at risk for conditions like diabetes, heart disease, or sepsis, even before symptoms appear.
Together, these technologies form a diagnostic engine that is continuously learning and improving. Machine learning in medicine is no longer just about analyzing what’s already wrong; it’s about anticipating what could go wrong next.
The Numbers Don’t Lie: AI vs. Human Accuracy
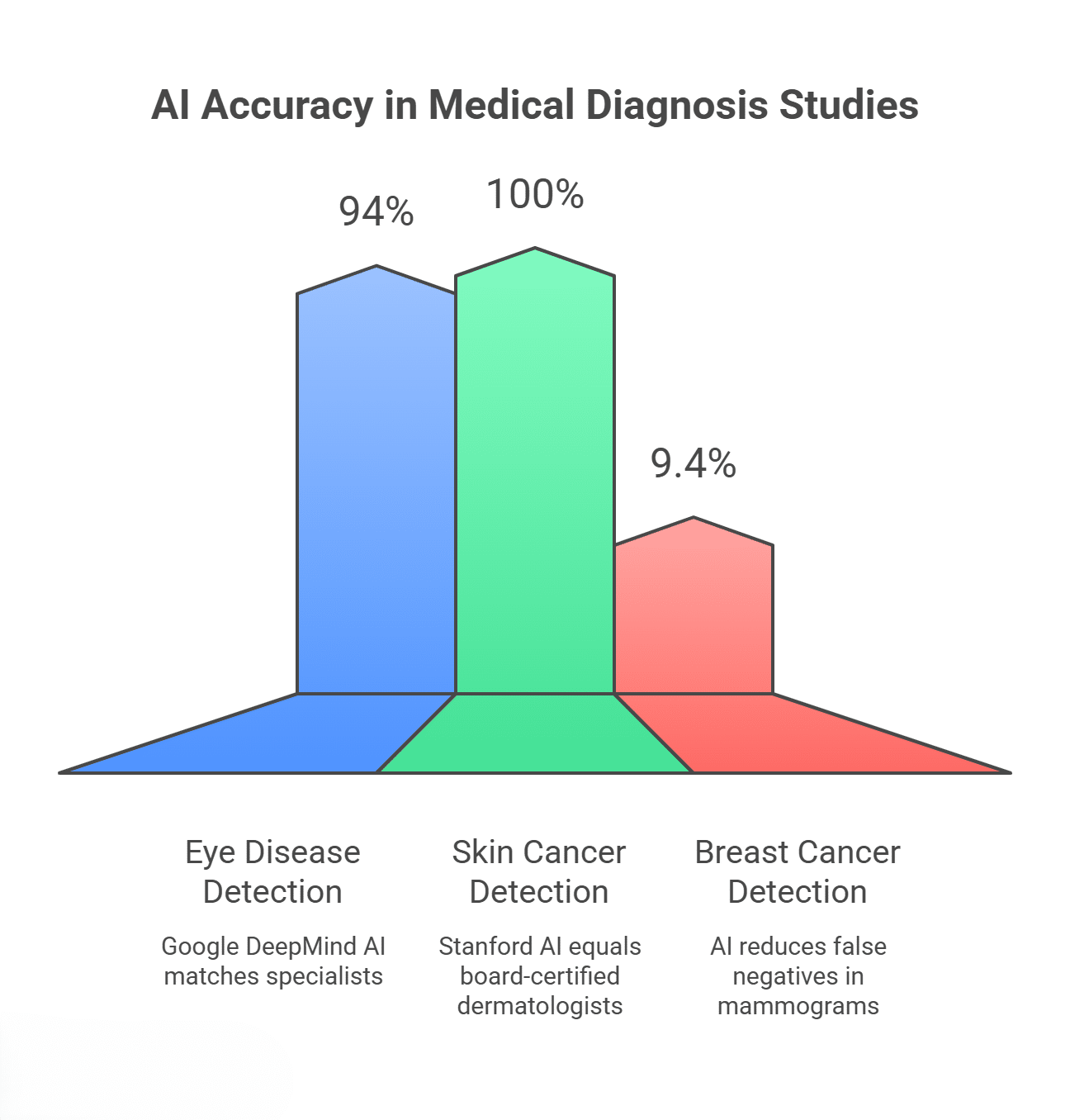
Numbers tell a compelling story about AI medical diagnosis accuracy.
A study in Nature Medicine found that an AI system diagnosed breast cancer. It achieved a higher level of accuracy compared to human radiologists using mammograms. It cut false negatives by 9.4% in the US test group.
In another study, Google’s DeepMind AI analyzed retinal scans and recommended correct referrals for over 50 eye diseases with 94% accuracy — matching the performance of world-leading eye specialists.
AI models trained on skin images can match or beat dermatologists. They are good at spotting skin cancer. A Stanford University study found that AI detects skin cancer. It does this with the precision of board-certified dermatologists.
These achievements are not isolated. AI in radiology, pathology, and cardiology often matches or surpasses human specialists.
But, raw accuracy only tells part of the story. AI medical diagnosis accuracy doesn’t try to replace human judgment. It aims to make it better. When doctors work with AI, they diagnose better than they could on their own.
Meet the AI Diagnosis Tools That Doctors Are Actually Using in 2026
It’s one thing to read about AI in theory. It’s another to see which tools are actually being used at the bedside.
Viz.ai is one of the leading AI platforms in stroke detection. It analyzes CT scans in real time and alerts specialists within minutes of identifying a potential stroke, dramatically cutting the time to treatment.
Paige.ai has received FDA clearance for AI-powered prostate cancer detection in pathology. It assists pathologists in identifying cancerous cells with higher consistency and speed.
Aidoc is a radiology AI platform used in over 1,000 hospitals worldwide. It flags urgent findings, like pulmonary embolisms and intracranial hemorrhages, so radiologists can prioritize critical cases first.
IBM Watson Health, though controversial in its early days, has evolved significantly. Its oncology tools now assist in matching cancer patients to clinical trials and treatment options based on their specific genetic profiles.
Did You Know? The global AI in healthcare market was valued at over $20 billion in 2023 and is projected to exceed $188 billion by 2030. These AI diagnosis tools aren’t replacing doctors’ decisions; they’re equipping them with better information, faster.
Is AI Diagnosis Too Good to Be True?
With all this promise, it’s reasonable to wonder: what’s the catch?
AI’s effectiveness hinges on the data it’s trained with. A model that focuses on one group, like lighter-skinned patients, may not help everyone. It could leave out others who need support. It may not work well for different groups. This is a recognized issue. Researchers have found racial and gender biases in AI diagnostic tools. This is especially true in dermatology and cardiology.
The “black box” decision-making presents another concern. Many deep learning models have trouble explaining why they mark a scan as abnormal. A diagnosis without a clear reason can be hard for doctors and patients to trust or defend in court.
Regulatory frameworks are still evolving. The FDA has approved many AI medical devices. But, oversight is still evolving. Issues around liability, data privacy, and clinical validation standards are being clarified worldwide.
These challenges shouldn’t deter us. AI is a powerful tool. It needs careful use, regular checks, and human oversight. As we look toward 2026, integrating AI into healthcare is crucial for meaningful transformation.
60% Faster, Significantly Cheaper: The AI Diagnosis Revolution
Speed and cost are two areas where AI is making a particularly dramatic impact.
Traditional diagnostic pathways can take days or weeks. A patient presents with symptoms, gets referred for imaging, waits for a radiologist’s report, and then waits again for a follow-up appointment. By that point, a treatable condition may have progressed.
AI compresses that timeline significantly. Studies suggest AI-assisted diagnosis can reduce diagnostic time by up to 60% in some specialties, particularly in radiology and pathology. That’s the difference between catching a tumor at Stage 1 versus Stage 3.
The cost savings are equally substantial. Faster diagnoses mean shorter hospital stays, fewer unnecessary tests, and earlier interventions that are less expensive to treat. A McKinsey report estimated that AI could reduce overall healthcare costs by 5–10% when deployed at scale, totaling tens of billions of dollars annually.
For patients in underserved communities with limited access to specialists, AI-powered diagnostic tools can provide a level of expertise that would otherwise be geographically or financially out of reach.
AI Is Not Replacing Doctors, It’s Making Them Superhuman
Here’s a concern worth addressing directly: will AI take doctors’ jobs?
The honest answer is no, at least not in any meaningful near-term sense. What AI is doing is fundamentally changing what it means to be a doctor.
Physicians who use AI can process more patients, catch more conditions, and make more confident decisions. A radiologist supported by AI can review twice as many scans without sacrificing accuracy. A general practitioner with an AI-powered clinical decision tool can flag rare conditions they might not have encountered in years of practice.
Think of it this way: calculators didn’t eliminate mathematicians; they made them more productive. AI in medicine works the same way.
The World Health Organization has noted that the world faces a projected shortfall of 10 million healthcare workers by 2030. AI won’t replace those workers, but it can stretch the capacity of the ones we have, ensuring that fewer patients fall through the cracks.
The doctors thriving in 2026 aren’t those who resist AI. They’re the ones who’ve learned to work with it.
Real Patient Stories: When AI Caught What Doctors Missed
Behind the data, real lives are changed. In a Johns Hopkins study, AI analyzed mammograms and flagged early breast cancer missed by five radiologists, spotting subtle signs like microcalcifications.
In the UK, DeepMind AI on eye scans caught diabetic retinopathy in GP patients initially overlooked, with 95% sensitivity, enabling treatment before vision loss.
A Singapore trial uses AI on blood/scan data for fatigue-linked heart risks, diagnosing faster than standard consults and mirroring cases of breathlessness missed early.
These aren’t hypotheticals; they’re patients reuniting with families thanks to AI’s pattern-spotting edge.
What 2027 and Beyond Looks Like
The pace of AI development in healthcare shows no sign of slowing down.
Multimodal AI, systems that can simultaneously analyze imaging, lab data, genetic information, and clinical notes, is expected to become mainstream within the next two to three years. This will allow for a far more comprehensive view of patient health than any single data source can provide.
Wearable technology will feed real-time health data into AI diagnostic platforms, enabling continuous monitoring and early warning systems for conditions like arrhythmia, hypoglycemia, and early-onset neurological disorders.
The integration of AI in healthcare with genomic medicine is particularly exciting. As genetic sequencing becomes cheaper and more widespread, AI will help decode the complex interplay between genetics and disease risk, enabling truly personalized preventive care.
Regulatory bodies are also maturing. Clearer frameworks for AI transparency, bias testing, and clinical validation are being developed globally. By 2027, the question won’t be whether AI belongs in medicine; it’ll be how to use it most responsibly.
AI as the Doctor’s New Best Friend
The evidence is clear: AI is not the future of medical diagnosis; it’s already the present.
AI medical diagnosis in 2026 is having a big impact. It helps detect cancer earlier and flags strokes faster. Also, it reduces costs and expands access in underserved communities. The effects are real, measurable, and growing. Patients are receiving more accurate diagnoses. Doctors are making better-informed decisions. And healthcare systems are becoming more efficient.
Researchers, clinicians, and policymakers are facing real challenges like bias, explainability, and regulation. They understand the stakes, so they are addressing these issues head-on.
The most important shift isn’t technological. It’s cultural. Medicine is starting to see AI as a helpful partner, not a threat. It helps doctors improve their skills. It makes diagnoses clearer, and keeps patients safer.
The stethoscope transformed how doctors listened to the body. AI is transforming how they understand it. That’s not a disruption; it’s progress.
Common Questions About AI Medical Diagnosis (2026 Edition)
Can I use AI to diagnose myself at home?
Several consumer AI diagnosis tool and symptom checkers are available, but they are not a substitute for professional medical advice. Apps like Ada and Buoy Health can help you understand your symptoms and decide whether to seek care, but they lack access to your full medical history and cannot perform clinical tests. Always consult a licensed healthcare professional for any diagnosis or treatment decision.
How accurate is AI compared to a human doctor?
It depends on the specialty and the task. In specific areas like radiology and pathology, AI has matched or exceeded human specialist accuracy in controlled studies. However, AI performs best when used alongside a doctor, not in place of one. The combination of AI precision and human clinical judgment consistently outperforms either working alone.
Who is responsible if an AI makes a wrong diagnosis?
This is an evolving area of medical and legal practice. In most jurisdictions, the treating physician retains responsibility for the final diagnosis. AI is considered a decision-support tool, not a decision-maker. Hospitals and AI vendors also carry liability depending on how the tool was deployed and whether it was used within its approved scope.
Is my medical data safe when processed by an AI?
Reputable AI healthcare platforms are required to comply with data protection regulations like HIPAA in the US and GDPR in Europe. Your data is typically anonymized before being used to train or run AI models. That said, data privacy remains an active concern, and it’s reasonable to ask your healthcare provider how your information is being used.
What are “false positives” and “false negatives” in AI?
A false positive is when AI incorrectly flags a condition that isn’t there, for example, identifying a benign mass as cancerous. A false negative is the opposite: missing a condition that is present. Both carry risks. In AI diagnostics, researchers work to minimize false negatives (missed diagnoses) especially in life-threatening conditions, while keeping false positives low enough to avoid unnecessary patient distress or procedures.
Can AI detect diseases earlier than traditional methods?
Yes, and this is one of its most significant advantages. AI can identify subtle patterns in imaging, blood work, and genetic data that may not yet produce visible symptoms. Early detection of conditions like cancer, diabetic retinopathy, and cardiovascular disease can dramatically improve treatment outcomes and survival rates.
Will AI make my healthcare more expensive?
In the long run, most evidence suggests AI will reduce costs rather than increase them. Faster, more accurate diagnoses lead to earlier treatment, fewer unnecessary tests, and shorter hospital stays. While the initial investment in AI infrastructure is significant, the downstream savings for healthcare systems and patients alike are projected to be substantial.


Leave a Reply